We need to protect the elderly in South Africa from COVID-19
07 May 2020 | Story Gabrielle Kelly. Photo Wikimedia Commons. Read time 6 min.
University of Cape Town (UCT) post-doctoral research fellow Gabrielle Kelly comments on the challenges facing older people in the wake of the COVID-19 pandemic.
The South African Older Persons Act promises to protect and empower the elderly, but in reality, the contribution of older people to society is often overlooked and their needs neglected. This is particularly notable in our overburdened health system where younger populations are prioritised in terms of budget allocation, service provision is poorly suited to older people’s complex health needs, and there is a severe lack of geriatric expertise among health professionals.
Given the Covid-19 pandemic, we can no longer sideline or ignore older people. Older adults are at significantly greater risk of complications from the virus and case fatality rates increase significantly with age due to reduced immunity and the increased likelihood of existing chronic disease. This has been demonstrated in the Chinese data and, most recently, in Italy where 82% of the 827 deaths that had occurred by 11 March 2020 fell into the 60-plus age category.
The experiences of countries with more advanced spread of the disease show how quickly the virus can spread and how much pressure it can place on health systems. These countries do not face the additional burdens of high rates of TB and HIV, which are expected to add significant complexity to managing the disease in the South African context. Everywhere, but particularly in a country as unequal and burdened by disease as South Africa, there is a critical need to examine how the structure of our society and economy will shape this crisis and impact on vulnerable groups such as the elderly.
South Africa has the largest population of older people in Africa (9% according to Stats SA’s 2019 mid-year population report) and about 40% of the older population in South Africa is poor. Medical aid coverage rates are low, with about 80% dependent on the public health system.
While nursing homes can (and hopefully will) restrict access to the public to protect residents and caregivers vulnerable to the virus, the limited availability of long-term care facilities for the poor means that many older people in community settings with already significant unmet care needs are likely to be exposed to the virus via other household members who struggle to heed calls to self-isolate. While wealthier South Africans can afford to manage their contact with others, reliance on public services, crowded living conditions, use of public transport and inflexible work arrangements will make it difficult to manage the spread of the disease in poorer communities. This puts a large number of older people at significant risk.
At the beginning of April, more than 18 million people will gather in large numbers at South African Post Office and Sassa pay points, as well as merchant retailers, to receive their social grants. About 3.6 million of these beneficiaries are Old Age Grant recipients who will put themselves at significant risk of infection by collecting the monthly income on which they depend. Sassa needs to make provision for social grant payments to be staggered or for bank fees to be waived to encourage the use of ATMs as a means of accessing money and for strict hygiene protocol to be in place to manage the potential spread of the disease.
Older people, who need to regularly frequent public health facilities to receive chronic medication or receive care, are also at risk of exposure in these settings. Provision needs to be made for all older people to have their medication delivered to their homes and for wellness check-ups to be carried out by community health workers.
Older people play a critical role in our society. Most older people live in community settings, very often with younger kin. These intergenerational or skip-generational households rely heavily on grandparents to care for children or the sick and contribute significantly to household income through their pensions.
About 70% of older people in South Africa receive old age grants and there is a substantial body of research that shows how older women use this income to support unemployed and underemployed relatives. By doing so they significantly reduce levels of household poverty. Given high rates of unemployment, the illness or death of an older person in a household will have a significant impact on the financial status of coronavirus-affected households. The ability of parents of young children to work or seek employment will also be reduced if grandmothers are no longer able to care for their grandchildren.
To protect vulnerable groups such as the elderly, we not only need to think about how health and clinical responses are developed, but how all health and public services are delivered to ensure that measures are in place to limit older people’s and immune-compromised people’s exposure to the virus. All South Africans that are able to should self-isolate to protect those who are not able to and allow older people to continue to play their vital role in their families and communities.
Dr Gabrielle Kelly is a health and social policy researcher. She has a PhD in Sociology from UCT and is the Senior Researcher at the Samson Institute for Ageing Research.
Coronavirus Disease 2019 updates
COVID-19 is a global pandemic that caused President Cyril Ramaphosa to declare a national disaster in South Africa on 15 March 2020 and to implement a national lockdown from 26 March.
UCT is taking the threat of infection in our university community extremely seriously, and this page will be updated regularly with the latest COVID-19 information. Please note that the information on this page is subject to change depending on current lockdown regulations.
Frequently asked questions
Daily updates
Campus communications
2020
Resources
Video messages from the Department of Medicine
Getting credible, evidence-based, accessible information and recommendations relating to COVID-19
The Department of Medicine at the University of Cape Town and Groote Schuur Hospital, are producing educational video material for use on digital platforms and in multiple languages. The information contained in these videos is authenticated and endorsed by the team of experts based in the Department of Medicine. Many of the recommendations are based on current best evidence and are aligned to provincial, national and international guidelines. For more information on UCT’s Department of Medicine, please visit the website.
To watch more videos like these, visit the Department of Medicine’s YouTube channel.
Useful information from UCT
External resources
News and opinions

As the COVID-19 crisis drags on and evolves, civil society groups are responding to growing and diversifying needs – just when access to resources is becoming more insecure, writes UCT’s Prof Ralph Hamann.
03 Jul 2020 - 6 min read Republished
The Covid-19 crisis has reinforced the global consequences of fragmented, inadequate and inequitable healthcare systems and the damage caused by hesitant and poorly communicated responses.
24 Jun 2020 - >10 min read Opinion
Our scientists must not practise in isolation, but be encouraged to be creative and increase our knowledge of the needs of developing economies, write Professor Mamokgethi Phakeng, vice-chancellor of UCT, and Professor Thokozani Majozi from the University of the Witwatersrand.
09 Jun 2020 - 6 min read Republished
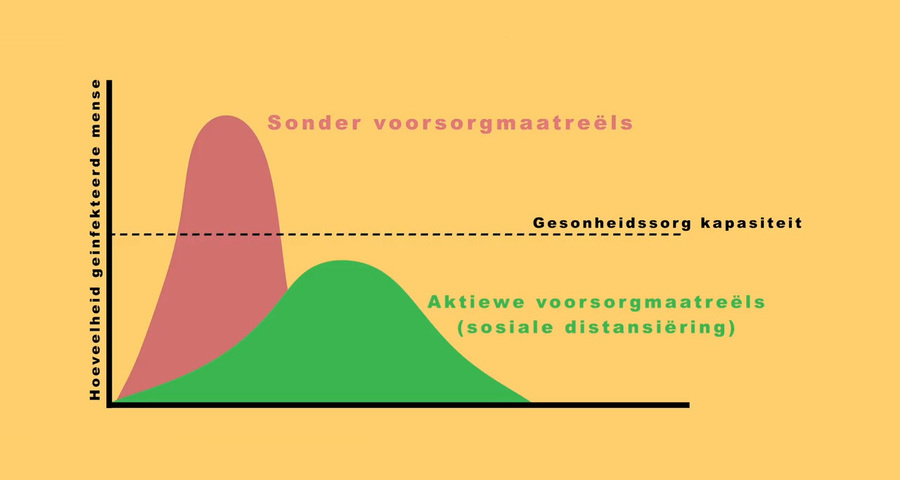
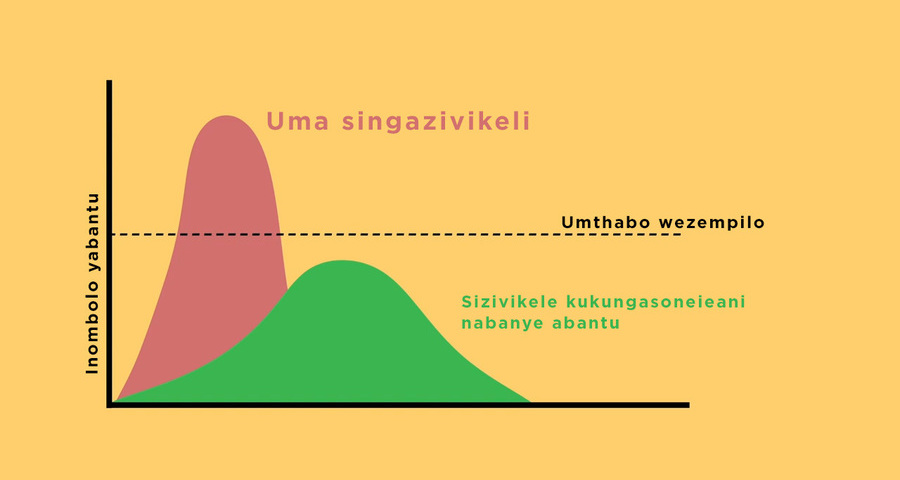
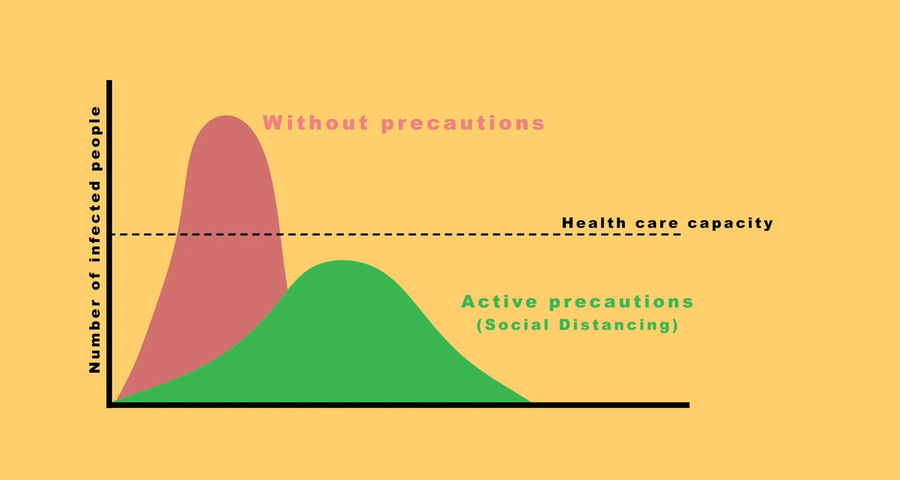
South Africa has been recognised globally for its success in flattening the curve, which came as a result of President Ramaphosa responding quickly to the crisis, writes Prof Alan Hirsch.
28 Apr 2020 - 6 min read RepublishedStatements and media releases
Media releases
Read more
Statements from Government
In an email to the UCT community, Vice-Chancellor Professor Mamokgethi Phakeng said:
“COVID-19, caused by the virus SARS-CoV-2, is a rapidly changing epidemic. [...] Information [...] will be updated as and when new information becomes available.”
We are continuing to monitor the situation and we will be updating the UCT community regularly – as and when there are further updates. If you are concerned or need more information, students can contact the Student Wellness Service on 021 650 5620 or 021 650 1271 (after hours), while staff can contact 021 650 5685.