A ‘call to arms’ for African vaccine manufacturing infrastructure
18 August 2021 | Story Di Caelers. Photo Nana Kofi Acquah, Wikimeda. Read time 8 min.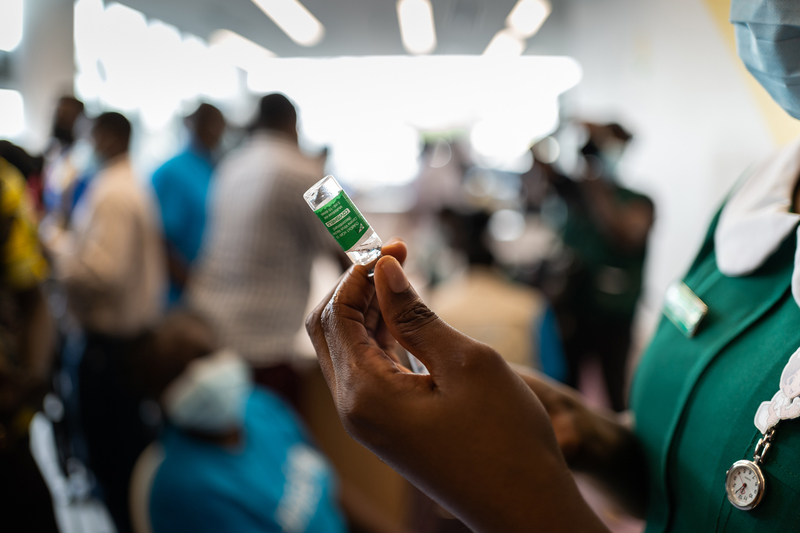
University of Cape Town (UCT) scientists have called for governments and private sector funders to join forces to urgently create the infrastructure to enable the transformation of local expertise into concrete vaccine manufacturing capability for Africa.
Their ‘call to arms’, contained in a recently published paper in Nature Reviews, entitled Prospects for SARS-CoV-2 diagnostics, therapeutics and vaccines in Africa, sounded the alarm early on in the COVID-19 pandemic.
While the onset of the pandemic prompted unparalleled progress in the development of vaccines and therapeutics in many countries, the authors cautioned that it also highlighted the vulnerability of resource-limited African countries.
This lack of capacity, in the context of the global demand for immunisation against the virus, “will further delay the availability of vaccines in the region”, they forecast – a reality that is playing out now as the COVAX Facility and the World Health Organization call on high-income countries to donate excess vaccines to their low-income neighbours.
Africa at the back of the queue
The announcement in July of a partnership between Pfizer and the Biovac Institute in Cape Town, to produce the Pfizer-BioNTech COVID-19 vaccine, created enormous excitement. But Emmanuel Margolin, the UCT postdoctoral scientist who was the lead author on the paper, says much more is needed to address the imbalance.
“The intention of this paper, published in a high-level journal, was to draw attention to the lack of vaccine manufacturing capacity in Africa. We can’t say that this pandemic was totally unexpected, even if no one expected the scope that we’re now seeing, yet we were caught napping,” he comments.
“There have been talks about establishing manufacturing capacity, but here we are more than a decade later, still completely reliant on other countries for essential medicines and vaccines.”
“We had multiple wake-up calls; during the 2009 H1N1 influenza pandemic a local shortage of vaccines resulted in limited supplies being provided for countries in the region. There have been talks about establishing manufacturing capacity, but here we are more than a decade later, still completely reliant on other countries for essential medicines and vaccines.”
Right now, Margolin points out, African countries are pretty much at the back of the queue, for multiple reasons that include an absence of manufacturing capacity.
His work straddles the Division of Medical Virology in UCT’s Department of Pathology, the university’s Institute of Infectious Disease and Molecular Medicine, the Biopharming Research Unit in the Department of Molecular and Cell Biology, and the Department of Integrative Biomedical Sciences.
A concerning reliance on developed countries
In the paper, he and his co-authors - Associate Professor Wendy Burgers, Professor Edward D. Sturrock, Professor Marc Mendelson, Dr Rosamund Chapman, Dr Nicola Douglass, Professor Anna-Lise Williamson and Professor Edward P. Rybicki - highlight vaccine and diagnostic production platforms that are being developed in Africa, and which can be translated into clinical development through appropriate partnerships for manufacture.
Infrastructure limitations, the authors wrote, “constrain the development of prophylactic vaccines and therapeutic interventions, which results in a concerning reliance on developed countries”.
They highlight the “considerable expertise in preclinical vaccine development” that is available in academic institutes, saying that vaccines could be manufactured on contract for clinical trials in much the same way as occurred for the South African AIDS Vaccine Initiative.
Commenting on the content, Margolin says it is extremely important to remember that what happens in the rest of the world isn’t always easily applicable to Africa, which will always have to pay attention to how best to use available resources in order to have the most impact.
Without Africa developing its own independent vaccine manufacturing capacity, the work cannot be translated into actual jabs in arms.
“At the time of writing, we were thinking about how we could apply our vaccine development work to SARS-CoV-2 to show, in principle, that we have the expertise to develop vaccines, even if we don’t have the infrastructure to make them at scale,” he explains, adding that his main focus area is how to make the surface proteins of viruses in plants, as a cheap, scalable source of vaccines.
But without Africa developing its own independent vaccine manufacturing capacity, the work cannot be translated into actual jabs in arms. And this capacity, Margolin stresses, must apply to the continent as a whole rather than to individual countries.
Capacity through the entire vaccine production process
Addressing latest advances towards so-called fill-and-finish capability in several African countries, including South Africa, Margolin acknowledges that this is a step in the right direction. Fill-and-finish refers to South Africa, for example, being utilised by pharmaceutical companies as a third party to fill vials with vaccines, and to finish off the packaging process to prepare these for distribution.
While it’s not end-to-end manufacturing, he says it does give countries leverage and access to vaccines to which they wouldn’t have previously had access.
“We must develop technologies that are suited to the needs of the continent.”
“But what we really need is independent capacity that goes the whole way through the vaccine production process, right from manufacturing the drug substance ourselves, to taking responsibility for all the vialing and distribution.”
It’s important that such technologies are suited to the needs of the entire continent, and not tailored to specific countries, he adds. “We must develop technologies that are suited to the needs of the continent if we are to be able to stop drawing attention, as we do in our paper, to the extreme vulnerability of African countries.”
Africa may be able to catch up in terms of vaccines for COVID-19, but Margolin is concerned about the continent having the necessary capacity to respond to the next pandemic.
“What are we going to do in five, 10 or 20 years when we have a similar situation? Will we be ready to act?
“We must also be aware that we’re looking at 1.2 billion people on the continent. That a whole lot of doses for which we need to be prepared,” he stresses.
 This work is licensed under a Creative Commons Attribution-NoDerivatives 4.0 International License.
This work is licensed under a Creative Commons Attribution-NoDerivatives 4.0 International License.
Please view the republishing articles page for more information.
Research & innovation





































