SA ‘falling short’ on HIV prevention goals
14 June 2019 | Story Supplied. Photo UCT Archives. Read time 6 min.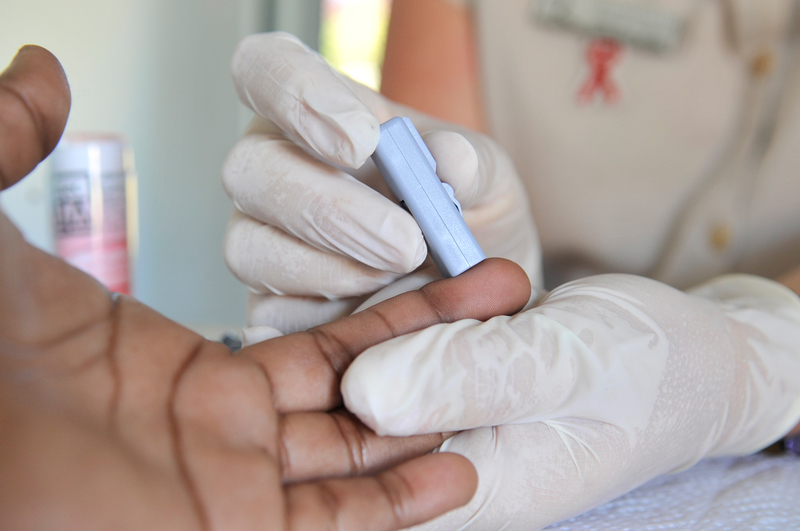
South Africa’s struggle to meet its HIV treatment coverage goals, combined with strong evidence of reduced condom use, is key to the slow progress in achieving reduced HIV incidence, according to a new study released by the University of Cape Town (UCT) yesterday
This is despite significant improvements in HIV testing rates and increased HIV suppression in patients who are receiving antiretroviral treatment (ART), according to UCT epidemiologist and actuary Dr Leigh Johnson.
Johnson’s study is based on the Thembisa model, a mathematical model for which he was a lead developer. It is calibrated to the latest HIV survey data, mortality data and HIV data from health services, as supplied by the national Department of Health.
Presenting the findings at the South African Aids Conference in Durban on 13 June, he unpacked the two factors he said are hampering progress towards the country’s HIV incidence reduction target.
“First, ART coverage is lower in South Africa than in other southern African countries, and we need to do better in linking HIV-diagnosed individuals to care, and retaining them in care.
“Secondly, there is increasingly strong evidence of reductions in condom use, relative to the levels we would expect in the context of high levels of HIV diagnosis,” Johnson said.
He also raised a red flag around adolescent girls and young women aged between 15 and 24, who account for 31% of all sexually-acquired HIV.
“[This is] a group that requires special attention.”
HIV prevalence data
Johnson’s Thembisa model was first published in 2014, and is regularly updated. The latest version, Thembisa 4.2, takes into account a number of new data sources that were not included in previous versions. Examples include HIV prevalence data from the 2016 Demographic and Health Survey, and recorded numbers of deaths of children.
However, the study does point to some success stories – such as KwaZulu-Natal, the province with the most severe HIV epidemic, which has succeeded in reducing its total annual number of new infections by 49% over the period from 2010/11 to 2017/18.
“There have also been substantial declines in AIDS mortality, with a 50% reduction in the annual number of AIDS deaths in South Africa.”
Thembisa also estimates that the annual number of new infections in children declined from 29 000 in 2010/11 to 13 000 in 2017/18 – a 55% reduction.
There have also been substantial declines in AIDS mortality, with a 50% reduction in the annual number of AIDS deaths in South Africa. These declined from 161 000 in 2010/11 to 80 000 in 2017/18.
Johnson said that although HIV prevalence is higher in women, more infected men are dying from AIDS.
“For example, over the 2017/18 period women accounted for 62% of new HIV infections in adults, but men accounted for 52% of adult AIDS deaths.
HIV testing uptake
“This difference is in part because of differences in uptake of HIV testing and treatment,” he explained.
In 2018, Thembisa estimated that 58% of HIV-positive men in South Africa were on ART, compared to 64% of women.
“While South Africa has been making progress towards reducing HIV incidence, there is concern that the progress is too slow.”
Johnson pointed out that while South Africa has been making progress towards reducing HIV incidence, there is concern that the progress is too slow.
From mid-2017 to mid-2018, Thembisa estimated that there were 249 000 new HIV infections, a 36% reduction on the 388 000 new infections that occurred from mid-2010 to mid-2011. This fell significantly short of the UNAIDS target of a 75% reduction in the annual number of new infections between 2010 and 2020.
Johnson said that to meet this target, the country would need to reduce its annual number of new infections to fewer than 100 000 within the next year, which appeared unlikely in light of the slow pace of decline to date.
Overall, the Thembisa model estimates that in 2018 there were 7.39 million South Africans – or 12.9% of the population – living with HIV. Of these, estimates were that 90.5% knew they were HIV-positive, 68.4% of those diagnosed were on ART, and 88.4% of those receiving treatment had a viral load equivalent to the UNAIDS definition of viral suppression (which means the virus cannot be transmitted to sexual partners).
The UNAIDS target is to get 90% of HIV-positive people diagnosed by 2020, with 90% of those diagnosed with HIV on ART, and 90% of ART patients virally suppressed.
Johnson said that while South Africa is performing well in respect of the first and third targets, it “is still a long way from reaching the (ART coverage) target”.
 This work is licensed under a Creative Commons Attribution-NoDerivatives 4.0 International License.
This work is licensed under a Creative Commons Attribution-NoDerivatives 4.0 International License.
Please view the republishing articles page for more information.
Research & innovation





































