Major advance in fight against TB
04 October 2018 | Story Supplied. Photo Supplied. Read time 4 min.
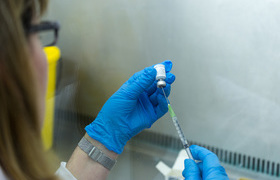
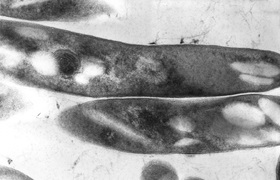
In a major advance for tuberculosis vaccine development, a multi-site trial across Africa has shown that the candidate tuberculosis vaccine M72/AS01Ecan prevent latent TB from progressing to active disease.
The South African Tuberculosis Vaccine Initiative (SATVI) and the Wellcome Centre for Infectious Diseases Research in Africa (CIDRI-Africa), tuberculosis research groups based in the Institute of Infectious Disease & Molecular Medicine at the University of Cape Town (UCT), are two of 11 sites in Kenya, South Africa and Zambia where the study is conducted.
“We have shown, for the first time, that a protein subunit vaccine can prevent progression to active TB in people who are already latently infected with the TB bacillus at the time of vaccination,” said Professor Mark Hatherill, director of the South African Tuberculosis Vaccine Initiate (SATVI).
The study is sponsored by the global healthcare company GSK, and conducted in partnership with Aeras, a non-profit organisation dedicated to developing vaccines against tuberculosis.
The results, published recently in the prestigious New England Journal of Medicine, detailed the findings of the ongoing Phase 2b clinical trial that is testing the candidate vaccine. The interim analysis showed that M72/AS01E significantly reduced incidence of pulmonary TB disease in HIV-negative adults already infected with latent TB at the time they were vaccinated.
The researchers said the results demonstrate “an overall vaccine efficacy of 54%”, with varied response rates for different groups. The candidate vaccine also demonstrated an “acceptable safety and reactogenicity profile”.
Leading cause of death
TB is the leading cause of death through infectious disease worldwide, and represents a significant public health threat with 1.6 million attributable deaths globally in 2016. In South Africa, the estimated incidence of TB is 781 per 100 000 people.
In addition, the World Health Organization estimates that a quarter of everyone worldwide has latent TB, with the potential for that dormant TB to progress to active disease in specific circumstances. The increasing prevalence of multi-drug resistant strains further complicates the picture.
“We are thrilled that a new generation TB vaccine candidate can prevent progression to active TB disease.”
There is currently no available TB vaccine with proven, consistent efficacy in adults, but Associate Professor Thomas Scriba, SATVI deputy director, said these findings offer significant hope.
“We are thrilled that a new generation TB vaccine candidate can prevent progression to active TB disease,” he said, adding that the study lays the foundation for the next step.
“That is to determine what this protective immune response looks like so that we can improve TB vaccines even further.”
CIDRI-Africa’s Professor Robert Wilkinson called the results intriguing and highly encouraging, pointing to the fact that the major task now is to analyse samples collected from the trial to look for clues of how “we might do even better”.
The study involved 3 573 HIV-negative adults who were followed for two years to detect evidence of pulmonary TB disease.
The final analysis, including all efficacy, safety, reactogenicity and immunogenicity data, will be performed next year after all participants have been followed up for a full three years.
 This work is licensed under a Creative Commons Attribution-NoDerivatives 4.0 International License.
This work is licensed under a Creative Commons Attribution-NoDerivatives 4.0 International License.
Please view the republishing articles page for more information.