Sub-Saharan Africa in desperate need of clinical haematologists
06 May 2021 | Story Niémah Davids. Photo Pixabay. Voice Neliswa Sosibo. Read time 6 min.
Sub-Saharan Africa faces a dearth of clinical haematologists. This urgently necessitates that more medical professionals embrace this branch of medicine and receive adequate training to specialise in this scarce skills area.
The Division of Haematology at the University of Cape Town (UCT) and Groote Schuur Hospital, headed by Professor Vernon Louw, is leading the way in this regard. The division, based in UCT’s Department of Medicine, is on a mission to train African clinical haematologists and boost the alarmingly low number of specialists on the continent who are equipped to help treat and manage blood disorders.
According to Professor Louw, the World Health Organization (WHO) recommends that all countries have at least one clinical haematologist for every 100 000 people. That means that South Africa, with a population of almost 60 million people, needs about 600 haematologists to meet the WHO target. But the country is nowhere near that total.
“Last [time] a proper calculation was done, we had 50 clinical haematologists in South Africa.”
“Last [time] a proper calculation was done, we had 50 clinical haematologists in South Africa. Since then, a few have retired, and others have opted to go and work overseas. So right now, as we speak, we have fewer than 30 clinical haematologists in the country,” Louw said.
Simplifying haematology
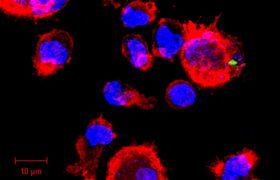
Haematology is the branch of medicine that studies and treats blood disorders and conditions that affect the bone marrow, the spongy tissue inside the bone that contains stem cells. Stem cells can develop into red blood cells, which carry oxygen through the body.
It’s for this reason that clinical haematologists also study and treat diseases that affect the stem cells. These include several cancers of the blood such as leukaemia, myeloma and lymphoma, and other diseases that are not necessarily cancer but that may lead to bone marrow failure, which causes an over- or underproduction of blood cells.
In essence, Louw explained, haematologists help to ensure that the cells in the body are optimised and that they work effectively. The cells include red blood cells – they carry oxygen to the body, white blood cells – they fight infection, and blood platelets – they protect the body from bleeding.
“If you have too few platelets you will bleed; if you have too many you will clot. If you have too few white cells, you’ll get infections all the time and if you have too many that’s usually an indication of leukaemia. If you have too few red cells then you’re anaemic,” he said.
“Basically, haematology deals with all these abnormalities of cells that are either too low or too high and sometimes we see combinations of high and low cell counts in the same patient, which is what makes it so interesting.”
Scarce skills area
The haematology clinic at Groote Schuur Hospital, UCT’s teaching hospital, consults with more than 12 000 patients annually. And while UCT is privileged to have a division solely dedicated to studying blood disorders, other universities in the country are not so lucky. Louw said that some medical schools have only one clinical haematologist and others have none. Yet, he stressed, this field of study is as important as any other branch of medicine.
In other parts of sub-Saharan Africa, the situation is no better. Angola, Namibia and Botswana do not have a single clinical haematologist between them, while Malawi and Zimbabwe have just one each, both of whom were trained in South Africa.
“Now, if you thought we had it bad, this is the sort of context that sub-Saharan Africa is currently facing.”
“Now, if you thought we had it bad, this is the sort of context that sub-Saharan Africa is currently facing. The main reason for it is because of a lack of training opportunities. There is a very big need for training haematologists on the continent and it’s one of the things we’re focusing on here at UCT,” he said.
On-site training
In the past, Louw said, the division spearheaded a number of outreach programmes in African countries to help train haematologists. But the approach wasn’t successful. “We’d go there for a week or two and do some training, but it was like a hit-and-run. It didn’t work very well, and we needed to come up with another plan,” he said.
Subsequently, on-site training came to mind. He and his team developed training programmes and recruited haematology registrars to further their studies in the field in Cape Town.
“We decided to let people come here and study here and then return home to their countries with the knowledge and skills to do everything they need to do. That’s a far better option,” Louw said.
Currently, he and his team are training several registrars from Zimbabwe and Sudan who will return to their home countries to practice there. Meanwhile, the number of trainees at the haematology clinic at Groote Schuur Hospital is increasing slowly.
Until recently the centre had just one or sometimes two trainees sub-specialising in clinical haematology. But that number has since increased to five, and an additional five candidates have approached the clinic for training. There’s more good news: Another three clinicians are also waiting to start their training programmes at the end of 2021 or during the first half of 2022.
“We are making inroads in this very scarce skills area.”
“This is very exciting, and it shows that we are making inroads in this very scarce skills area, which is so important. And even though funding remains our biggest challenge, we are optimistic that by lobbying government, this will change,” he said.
“We are on a mission to address this and drastically boost figures for the continent.”
 This work is licensed under a Creative Commons Attribution-NoDerivatives 4.0 International License.
This work is licensed under a Creative Commons Attribution-NoDerivatives 4.0 International License.
Please view the republishing articles page for more information.