Accelerate use of nuclear medicine as primary diagnostic, therapeutic modality
18 January 2024 | Story Niémah Davids. Photo Robin Thuynsma. Read time 7 min.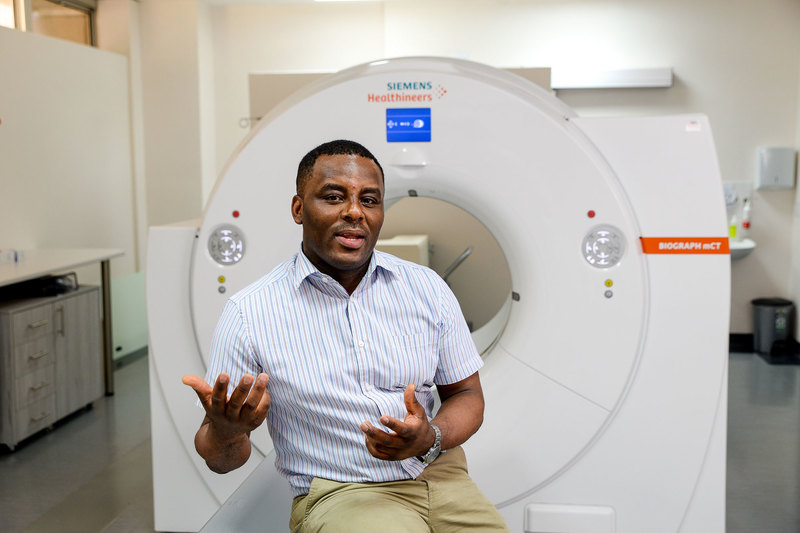
The field of nuclear medicine in South Africa is growing exponentially. And if it continues at this pace, health experts say this branch of medicine will revolutionise diagnostic and treatment options for patients with a spectrum of life-threatening, debilitating diseases, including cancer, cardiovascular disease, and neurodegenerative disorders.
According to Dr Stuart More, the acting head of the Division of Nuclear Medicine at the University of Cape Town (UCT) and Groote Schuur Hospital (GSH), the benefits of this area of medicine are twofold. With good success rates, it has been used as a treatment modality to fight various cancers and has demonstrated encouraging results with pain management and improving the quality of life for patients with debilitating conditions like rheumatoid arthritis (RA) – an autoimmune and inflammatory disease that causes excruciating pain and prevents patients from performing everyday tasks.
Speaking to UCT News from the cutting-edge nuclear medicine centre located in GSH’s New Main Building, Dr More said clinicians are working around the clock to ensure that this branch of medicine becomes easily accessible. To ensure it reaches patients in need, he stressed the importance of adopting a cross-disciplinary working model – leveraging other areas of medicine like oncology, cardiology and neurology to collectively establish the best treatment options for patients.
“This is a niche area of medicine that has the potential to assist patients in many ways, both with treatment and pain relief for different diseases.”
“This is a niche area of medicine that has the potential to assist patients in many ways, both with treatment and pain relief for different diseases. Yet, nuclear medicine is not routinely considered as a primary diagnostic or treatment option in South Africa, like elsewhere in the world. For the sake of our patients and their families, we need to change the narrative here,” he said.
At a glance
Simply put, nuclear medicine is a specialised area that uses radioactive material to determine how well organs and tissue are functioning (to enable a diagnosis). Once the diagnosis is made, radioactive substances are used to selectively treat the diseased area in the body using molecular precision, while simultaneously sparing healthy adjacent cells. This area of medicine combines chemistry, physics, mathematics, computer technology and medicine under one umbrella.
To study patients’ organ and tissue function, More said clinicians use technology imaging like the gamma camera, as well as the positron emission tomography (PET) and computed tomography (CT) scans. But not before patients are injected with a tiny amount of radioactive substance (radiopharmaceutical or radioactive tracer) first, to help clinicians reach an accurate diagnosis or assess the progress of various conditions – from malignant tumors, to characterising the extent of cardiovascular disease.
“It is an extraordinary branch of medicine that has yielded positive results for patients,” More said.
Notable results
Yet, despite its effectiveness, More said referring specialists don’t recommend nuclear medicine as the primary diagnostic or treatment go-to.
“In South Africa, nuclear medicine therapy is not the first port of call. It often comes in right at the end when other treatment modalities have been exhausted as the standard of care. What this means is that if someone is diagnosed with metastatic prostate cancer, they will go through all the traditional cancer-treating modalities first. And only once those prove to be ineffective, will nuclear medicine therapy be considered as a possible alternative,” he said.
More and his colleagues at GSH have been at the forefront of effecting this change, which, he added, starts by proving the efficacy of nuclear medicine.
Impactful treatment modality
To date, he said, clinicians at GSH have witnessed the treatment’s effectiveness with prostate and thyroid cancer, neuroendocrine tumours, and, more recently, with a patient with terminal brain cancer. With the latter, More said, because all other treatment options had failed and the patient was given just days to live, his medical team opted to give nuclear medicine therapy a go. Thanks to its effectiveness, the patient could spend eight additional months with his family.
“We need to move towards introducing radioactive therapy as a primary treatment modality and not as a last resort.”
“With this patient, all treatment options had failed and together with his oncologist, we decided to give nuclear medicine a try. The patient sadly passed away, but things started to change when he started radionuclide therapy,” More said. “This is precisely why we need to advocate for patients to be brought in on diagnosis. We need to move towards introducing radioactive therapy as a primary treatment modality and not as a last resort.”
Currently, More’s goal is to mobilise other units within GSH to help him recruit a bigger selection of eligible patients who are willing to trial nuclear medicine. This, he said, also applies to non-oncology patients, especially those who suffer from chronic pain like RA.
“We are making giant strides, and we need to continue moving in this direction. Leveraging the skills and expertise of clinicians in other fields is necessary to get their buy-in and to demonstrate the treatment’s true effectiveness to patients. We want them [specialist clinicians] to get to a point where they recommend radioactive therapy to their patients even though it’s outside of their discipline,” he said.
Extending its reach
But to reach as many patients as possible requires a lot more than making these diagnoses and treatment options available at tertiary-level hospitals.
More said additional, well-equipped nuclear medicine centres should also be established at district-level hospitals across the peninsula. Currently, centres like his are restricted to tertiary hospitals like GSH and Tygerberg Hospital. But by extending its reach, more patients will benefit from the service and the demand for specialists will increase as well. This, he added, will contribute to building a pipeline of trained clinicians in this scarce skills area of medicine in the country.
“If we can get this right, it will be a big win for the well-being of our patients, as well as for clinicians who are hoping to train as specialists, but who are reluctant to do so now because there are no jobs. It’s a burgeoning field globally and is growing by leaps and bounds in South Africa. But we need manpower, and we need more centres to facilitate the work among our patients,” More said.
“All this requires work on multiple different levels, in academia, government and civil society. We can get it right if we make a concerted effort to place the well-being of our patients first.”
 This work is licensed under a Creative Commons Attribution-NoDerivatives 4.0 International License.
This work is licensed under a Creative Commons Attribution-NoDerivatives 4.0 International License.
Please view the republishing articles page for more information.