Grant supports neuroscience study of childhood tuberculous meningitis
14 February 2022 | Story Nobhongo Gxolo. Photo Karin Schermbrucker. Read time 6 min.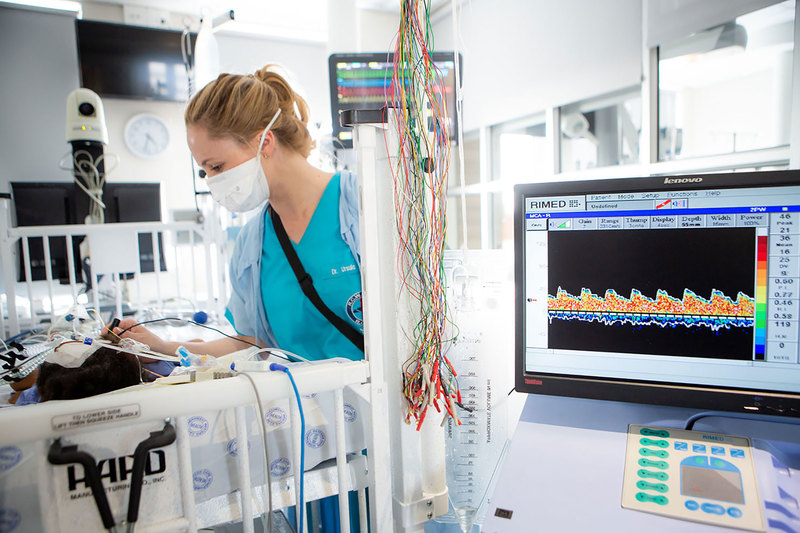
According to the WHO Global TB Report 2020, Africa accounted for 25% of the new global tuberculosis (TB) cases in 2019. In addition, South Africa ranks in the top eight countries with the highest global burden of TB disease. Africa is also the youngest continent with 60% of the population under the age of 25 years. Given the TB disease burden and the critical need to ensure brain health of the largest component of the continent’s population, African researchers are well placed to develop ways to optimise childhood brain health after TB infection.
Through a Wellcome Trust International Intermediate fellowship, Dr Ursula Rohlwink will study the brain infection – tuberculous meningitis (TBM) – in children. “We have the patients; we have the capacity, and with Wellcome’s support, we have the very real potential to do ground-breaking research that benefits our patients,” said Dr Rohlwink, who was recently awarded the fellowship. The grant will support her research costs and salary for the next five years while she develops exciting novel and clinically relevant data and acquires new skills.
Rohlwink’s work straddles the University of Cape Town’s (UCT) Department of Surgery at the Faculty of Health Sciences (FHS), UCT’s Neuroscience Institute (NI), and the Red Cross War Memorial Children’s Hospital (RCWMCH). The hospital houses the Paediatric Neurosurgery Unit, where the research enterprise Rohlwink works with is based. It is the leading paediatric neurosurgery unit on the continent and has one of the most advanced brain monitoring infrastructures globally.
“I hope to establish local capacity in terms of training and education of postgraduate students and [through] my ongoing involvement in building the infrastructure of the NI and the African Brain Child (ABC) Initiative, to stimulate the next generation of young neuroscience minds through public engagement, to contribute to the improved management of TBM through my work on the International TBM Consortium, and to continue to build the continental and international reputation of our neuroscience research.”
This fellowship is the third project focused on neuroscience to be awarded to UCT by the Wellcome Trust in the space of a year.
“This shows that Wellcome has put African neuroscience firmly on their radar and that they are committed to funding promising emerging African researchers who are driven to remain on the continent and to address important local questions.”
Damaging the developing brain has life-long consequences
Neuroscience-related pathologies – like brain infections, traumatic brain injury and brain cancer – represent an enormous yet under-studied burden of disease in Africa. Their impact is significant in children, as damage to the developing brain has life-long consequences.
“TBM is the most devastating form of TB disease because it can severely damage the brain. However, currently we don’t fully understand how this injury to the brain happens, how to detect it quickly enough, or how to treat it,” she said.
“The researchers will … examine a newly developed, highly sensitive blood-based test to identify brain injury early.”
The “Brain injury in paediatric tuberculous meningitis: mechanisms of injury and biomarkers of outcome” project will investigate the disease processes that damage the brain, to help the team develop treatments targeted to prevent them. The researchers will also examine a newly developed, highly sensitive blood-based test to identify brain injury early, while there is still time to prevent the injury from becoming permanent.
The team will use advanced brain imaging to investigate how TB infection disrupts brain networks and functional development in children. The fellowship “puts the brain at the centre of improving the survival and long-term function of children with TBM”.
Researchers dig deep to tap into resourcefulness
The national and international funding landscapes have been historically competitive for soft-funded researchers. This was a reality further exacerbated by the COVID-19 pandemic during which various international funders made significant cuts to their research budgets, especially for research based outside their borders.
“South African researchers have dug deep to tap into our resourcefulness.”
“For basic science researchers like me, who work within a clinical department, this was an even bigger blow. Permanent jobs or contract positions for non-clinicians are hard to find. Furthermore, lack of access to the clinical environment during 2020 set us back significantly in terms of patient recruitment and data collection, which made it challenging to continue translational research projects and to develop the data upon which grant applications are based.”
Rohlwink said South Africans have become adaptable and resilient through facing challenges like water shortages, load shedding, and now, a pandemic. So, “in that spirit, South African researchers have dug deep to tap into our resourcefulness.”
She said that the strength of her fellowship application lay in its strong translational aims. Rohlwink added that Professor Anthony Figaji, the head of Paediatric Neurosurgery at RCWMCH, established their research enterprise, the ABC Initiative, based on the principle of combining the clinic and the lab as equal parts of the solution to clinically relevant questions.
“Our team is made of both neurosurgeons and [neuro]scientists and this project will continue to rely heavily on our combined work. I am enormously grateful to have Prof Figaji, Drs Nqobile Thango, Nico Enslin, Jill Combrinck and Lisa Ungerer as my teammates. Our research unit exists in the broader ecosystem of the UCT Neuroscience Institute, directed by Professor Graham Fieggen, which fosters collaborations across various clinical and basic neuroscience research groups and supports us to become premier African and global neuroscientists.”
 This work is licensed under a Creative Commons Attribution-NoDerivatives 4.0 International License.
This work is licensed under a Creative Commons Attribution-NoDerivatives 4.0 International License.
Please view the republishing articles page for more information.