Anaesthesia & Perioperative Medicine tackles COVID challenges and high-risk procedures head-on
10 December 2020 | Story SUPPLIED. Read time 4 min.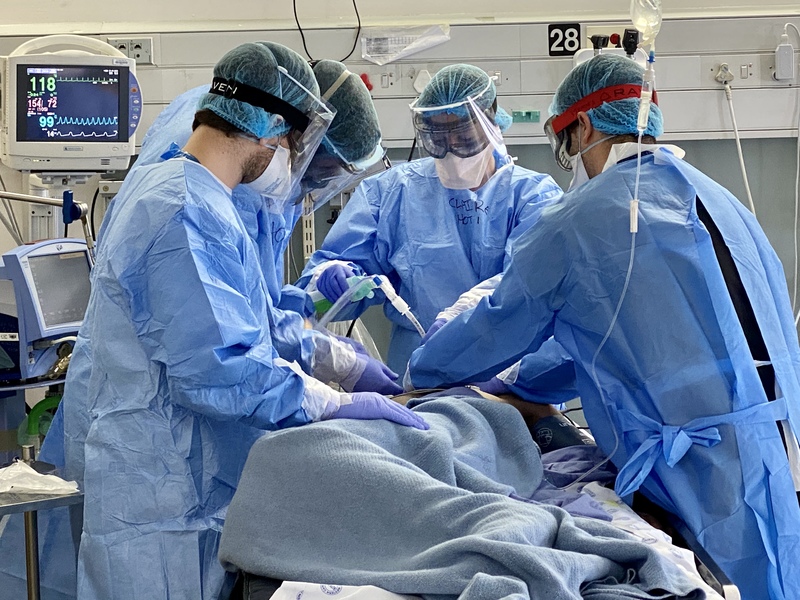
As the COVID-19 pandemic began taking its toll in Europe and the East, leaders in the Department of Anaesthesia and Perioperative (which incorporates the Division of Critical Care) stated that the predicted dramatic increase in critically ill patients would require significant escalation of intensive care services. In addition, the risky procedures of intubation and transfer of the sickest patients to intensive care units would place exceptional demands on the already overstretched ICU teams.
The combination of severity of disease and generation of aerosolized virus places patients and staff at high risk during intubation, stabilisation and transport. De-escalation of routine and elective surgery in the hospital in preparation for the pandemic allowed the Department to redeploy approximately half of its staff to COVID services, divided between expanding ICU capacity, and forming a dedicated COVID Anaesthesia and Airway Team. This team created a highly protocolized approach to safe intubation with defined roles, checklists and systems, and a safe operating theatre workflow for COVID-19 patients requiring surgery, which were subsequently adopted and openly propagated across the country by the SA Society of Anaesthesiologists.
Using existing experience in medical simulation, the team immediately began open training sessions for all hospital staff in correct use of personal protective equipment (PPE) for aerosol-generating procedures (AGPs), rapid intubation, and patient transfers. Specifically, this training was intentionally undertaken with in-situ simulation (in theatres, emergency departments and wards), and actively encouraged cross-disciplinary participation of staff in interchangeable roles.
.jpg) This strengthened collaboration between staff drawn to the COVID efforts across all departments, but also allowed systems testing and rapid improvement before the patient surge. All training materials (including a series of professionally-produced videos sponsored by SASA in collaboration with UCT), protocols and supporting documents were deliberately made open access and updates shared across the county (and world) in real time. In addition, a registry was immediately established to capture data surrounding the patients and their management, to feed into iterative debriefing and quality improvement, but also to support and form a foundation for future research.,
This strengthened collaboration between staff drawn to the COVID efforts across all departments, but also allowed systems testing and rapid improvement before the patient surge. All training materials (including a series of professionally-produced videos sponsored by SASA in collaboration with UCT), protocols and supporting documents were deliberately made open access and updates shared across the county (and world) in real time. In addition, a registry was immediately established to capture data surrounding the patients and their management, to feed into iterative debriefing and quality improvement, but also to support and form a foundation for future research.,
The formation of ad hoc teams at the bedside who were able to follow well-defined roles agnostic of the titles of the participants grew and strengthened the hospital, and the relationships of all involved. Remarkably, through strict adherence to infection control protocols and in contrast to international patterns the team has seen no COVID infections during this time. The data collected on clinical cases and practices has been collated and presented internationally, helping teams around the country and globe improve both their service to patients, and staff wellbeing.“From March to September, the COVID Anaesthesia and Airway Team managed more than 500 COVID cases, of which approximately half were intubations and transfers of critically ill patients to ICU, and more than a third cases requiring surgery.”
 This work is licensed under a Creative Commons Attribution-NoDerivatives 4.0 International License.
This work is licensed under a Creative Commons Attribution-NoDerivatives 4.0 International License.
Please view the republishing articles page for more information.










