DNA test uncovers hidden TB cases
09 February 2017 | Story by Newsroom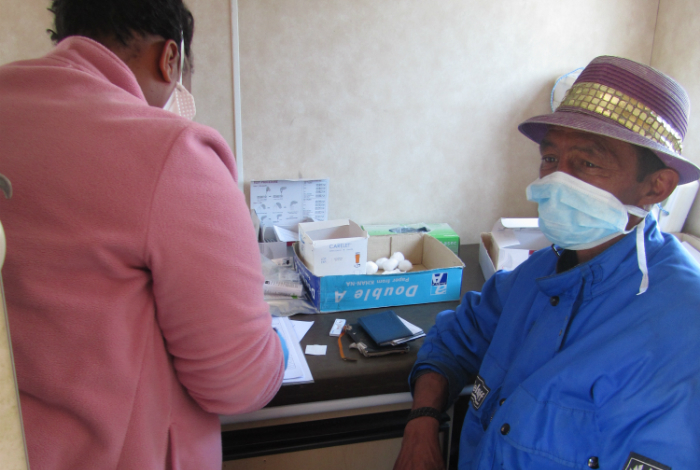
Tuberculosis has killed more than a billion people over the last two centuries. A new UCT-led study had the myriad undiagnosed cases of the highly infectious disease in its crosshairs.
It's estimated that 30–40% of TB cases globally are never diagnosed. Typically, TB tests happen only when prospective patients approach a clinic or hospital, which leaves many potential cases flying under the radar. This makes containing the spread of the highly infectious disease nigh impossible.
A study led by UCT's Dr Greg Calligaro and Professor Keertan Dheda, which was recently published in The Lancet: Infectious Medicine, flipped the come-to-us model on its head and brought a TB test to the people. The results were startling, but promising.
A DNA-based testing machine, called GeneXpert MTB/RIF, or simply Xpert, was placed in a mobile van along with a power generator and was driven to Langa, Cape Town, which is known to be a TB hotspot. Xpert was also taken to a clinic in Mabvuku, a suburb in Harare, Zimbabwe.
Megaphones and strategically placed advertising banners called people to come for a screening. In Mabvuku, prospective patients were driven to the clinic. Of the 2 261 people randomly selected for screening, 875 patients with suspected pulmonary TB were enrolled for diagnosis.
The results
Roughly half of these patients were randomly assigned to be tested by the new Xpert machine, which required a urine sample and a culture sample taken from the patient's sputum. The rest were tested the routine way, using smear microscopy and culture samples.
With all protocol observed, 53% more patients started treatment after being tested by Xpert than patients who had been tested using the standard smear microscopy approach, which is used in many countries where TB is endemic. This is possibly because smear-negative TB cases are responsible for 17–20% of all TB transmission, and the authors suspect that in communities with a high TB burden, like Langa, the transmission of smear-negative cases might be even higher.
Xpert-tested patients also initiated treatment sooner (nearly 50% sooner) than those tested the routine way.
This study, the first time that GeneXpert has been evaluated at the point of contact in a mobile van in sub-Saharan Africa, suggests that many more cases of TB can be detected with such a proactive approach. The potential knock-on effects on TB transmission gives the researchers hope that the spread of the disease could be limited as more and more patients, who might otherwise have gone undiagnosed, are identified and treated. This will, however, need further study.
“Our study shows the staggering burden of undiagnosed tuberculosis in the community in high burden settings, and reinforces the importance of intensified case finding as a pillar of tuberculosis control,” say the authors of the study.
Story Yusuf Omar. Photo Dr Virginia Buser.
 This work is licensed under a Creative Commons Attribution-NoDerivatives 4.0 International License.
This work is licensed under a Creative Commons Attribution-NoDerivatives 4.0 International License.
Please view the republishing articles page for more information.










