How an Ebola clinic works
28 October 2014 | Story by Newsroom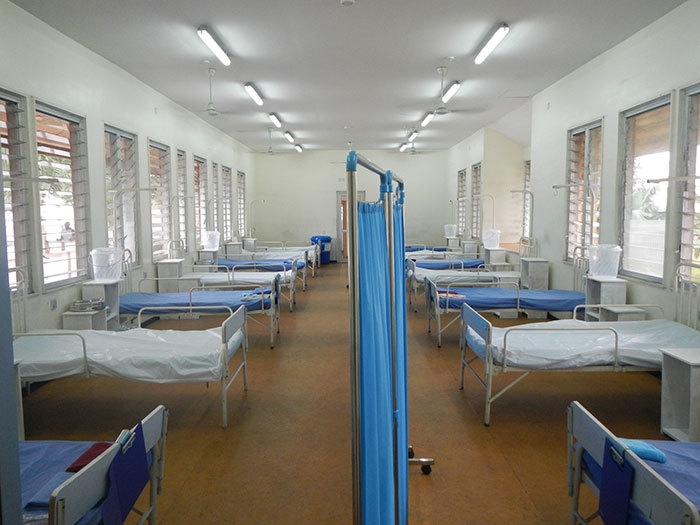
"So just think of the one who is about to die, trapped behind hundreds of walls sizzling with heat, while at the same time, there are all those people, on the telephone or in cafés ..." '“ The Plague, by Albert Camus.
Can you tell us who you were living with before you came here? The health promoter shouts across the fence.
Feeling uncomfortably self-conscious for drawing this patient to the feeding area to talk to him, I stand about seven metres away, in the blazing sun, shading my eyes to try to read the emotion in his face. He is middle-aged, and he lost his wife to Ebola three days ago. He cared for her while she was dying. He was brought in by ambulance to our treatment centre last night, with a fever.
We are trying to probe, very gently, whether there was anyone else who may have been in contact with him when he became sick. This is so that the health promotion and surveillance teams can follow up with the contacts to ensure that if they are in quarantine, they have sufficient food, drinking water, mattresses and soap for infection control; and to address the concerns of the community, and sensitise them to Ebola.
The man doesn't speak. Sitting on a chair, though his arms have the muscular definition of a hard-labourer, his body is limp, and shiny with perspiration. He remains silent, frowning slightly, trying to remember. 'My niece.' His eyes cloud over, and he looks away. I think he's overcome. 'Don't push it,' I say to the health promoter; and then, after asking the man if he needs anything, we thank him and walk away.
His story will probably be similar to those of the twelve others who were admitted as suspect cases last night. Some arrive in the ambulance, after a four-hour journey, and are too traumatised to speak. It's my job to enter each admission into the database, and to look for links between them, as well as to monitor the location from where they've come in order to identify potential new clusters of infection.
Every day, I follow the strict infection-prevention and -control procedures to enter the treatment site. The smell of chlorine is ubiquitous; as we enter, we wash our hands and then stand one-legged and wobble as each shoe is sprayed '“ both activities performed with chlorinated water, of different concentrations. Scrubs and boots are handed over, and changing into them is a challenge: nothing must touch the floor.
The treatment centre is divided into zones of risk; the low-risk area is where patient administrative work is carried out, by medical and clerical staff. This is where I encode my data, closely watching the patient and laboratory whiteboards for new admissions, the daily blood results, and the changes in status for each patient.
In the high-risk zone, medical staff move carefully and slowly around patients in a dozen tents that have been pitched in two rows of six, delineating the path and eventually the fate of the patient, using the fancy epidemiological terms 'suspect' and 'probable' '“ based on clinical diagnostic criteria, and then confirmed with a blood test, before leading either to convalescence or death.
For us, the priority is personal protection and safety. Continuous vigilance leads to obsessive hand-washing and keeping space between ourselves in order to apply the '˜no touch' mission policy. Actions need to be carried out carefully and slowly in order to prevent mistakes; any error has the potential to bring the whole team down.
He died today, three days after I spoke to him. I feel a short stab in my chest as I scan the death register and recognise his name. The medical staff tell me that he died doubled over in prayer, facing East. It was unexpected, and most probably instantaneous. Little is known about the pathology of this virus; death seems to strike suddenly at times.
 Kathryn Stinson has a PhD in Public Health and is an epidemiologist at the University of Cape Town. She has three children, two Great Danes and one very supportive husband. Kathryn writes in her personal capacity.
Kathryn Stinson has a PhD in Public Health and is an epidemiologist at the University of Cape Town. She has three children, two Great Danes and one very supportive husband. Kathryn writes in her personal capacity.
Photo of Kathryn Stinson and article were first published on GroundUp under a Creative Commons 4.0 License. Photo of isolation ward courtesy of Bryan Christensen under creative commons 2.0 license.
Read more:
Ebola: journey to a quarantined village
 This work is licensed under a Creative Commons Attribution-NoDerivatives 4.0 International License.
This work is licensed under a Creative Commons Attribution-NoDerivatives 4.0 International License.
Please view the republishing articles page for more information.