World Mental Health Day a local concern, too
07 October 2011 | Story by NewsroomMonday, 10 October, is World Mental Health Day.
It's a day that allows groups like the World Health Organisation (WHO), the World Federation for Mental Health and others to, as it does most other days, highlight concerns around mental health issues and, more specifically, the poor levels of treatment. The majority of low- and middle-income countries spend less than 2% of their health budget on mental health, for example, the WHO points out.

|

|
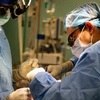
| Troubled minds: The majority of low- and middle-income countries spend less than 2% of their health budget on mental health. (Picture courtesy of the WHO/P Virot.) | Prime care: An international, UCT-led project, PRIME hopes to expand the coverage of mental health services. |
South Africa, too, has its worries. While there's plenty of policy and legislation, it hasn't always been implemented even-handedly around the country, points out UCT's Department of Psychiatry and Mental Health in a statement to mark World Mental Health Day (WMHD).
In the Western Cape, for example, representatives from the provincial Department of Health and academics have built strong collaborations, meet regularly and discuss research every WMHD, as they will do this year at Lentegeur Psychiatric Hospital in Mitchell's Plain. The province will also host the 2nd Summit of the Movement of Global Mental Health and the World Congress of the World Federation for Mental Health in October.
But as Charlene Sunkel, a mental health activist with the Central Gauteng Mental Health Society and who also lives with mental illness, experienced in Gauteng, not all provinces - or patients - are so fortunate. "I had numerous admissions to various state psychiatric hospitals, where in some of them I witnessed and experienced emotional and physical abuse," she says.
Problems, adds Sunkel, include stigma, long waiting times and lists, a shortage of medication, and distrust and discomfort among patients in the face of regularly rotating psychiatrists.
In response, mental health researchers have developed a model for implementing community mental health services in South Africa. For its part, UCT's Department of Mental Health and Psychiatry conducts extensive training of psychiatrists and mental health researchers.
This work and research is also being rolled out to other low- and middle-income countries. The UCT-based Centre for Public Mental Health, in one example, is spearheading the PRogramme for Improving Mental health care PRIME, a global research group of mental health experts and policymakers that includes the WHO, the Centre for Global Mental Health (incorporating the London School of Hygiene & Tropical Medicine and King's Health Partners in the UK), and health ministries and academic institutions in five low- and middle-income countries (Ethiopia, India, Nepal, South Africa and India).
PRIME's main goal is to expand the coverage of mental health services across those five countries.
 This work is licensed under a Creative Commons Attribution-NoDerivatives 4.0 International License.
This work is licensed under a Creative Commons Attribution-NoDerivatives 4.0 International License.
Please view the republishing articles page for more information.